Lu Molberg of Palm Springs is a firm believer in alternative medicine. Through research and pursuing treatments that aligned with her beliefs, Molberg became an informed health care consumer. Taking control of her health has been empowering, she said.
“You do have to have trust in health care,” said Molberg, “but most of all you have to have trust in yourself to make the right decisions.”
Now in her 70s, Molberg stays healthy by monitoring the energy aspects of her body, teaching t’ai chi and staying current on her health care appointments.
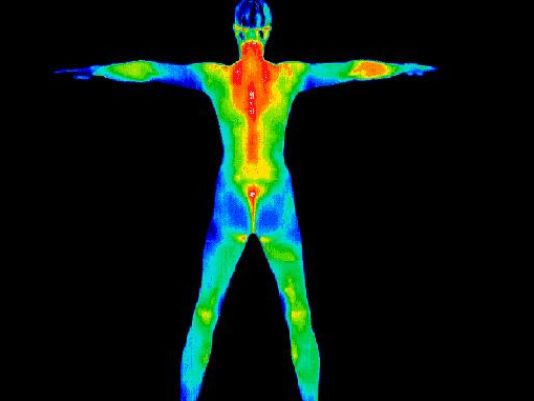
One practice that Molberg subscribes to is thermography — a non-invasive, full-body infrared scan that can help detect any changes in her body on a physiological level. Conventional practices like mammography have their place, but thermography, she said, is the path of least resistance.
“You’re able to relate to a person and not a machine,” Molberg said.
Thermography as a health screening does far more than map the different temperature changes of the human body; it can motivate people to lead a more prevention-based lifestyle.
“Thermography closes the clinical gap between when a person starts to leave their healthy state until that point when that have that something serious enough to be diagnosed,” said Dr. Hillary Smith, a level three certified clinical thermographer and chiropractor. “There’s all that time in between and that’s what thermography is looking at.”
Smith practices in Los Angeles but also visits the Optimal Health Center in Palm Desert to screen patients, and will be participating in a health discussion at Palm Desert Library on Monday.
So often associated with breast screenings, thermography can be used to screen the entire body.
“People have a thermal fingerprint,” said Smith. “Only a developing problem will change that thermal fingerprint.”
For example, said Smith, if a person were to get a splinter, an X-ray could see the piece of wood but would not detect inflammation or infection. Thermography can instead detect the changes in heat and any infection, but not the splinter itself.
In order to document and understand a person’s unique thermal fingerprint, two series of scans are completed three months apart, added Smith. A base line is created and future appointments help monitor any possible changes.
After the screening, the images are sent to medical doctors who are thermologists for interpretations, and if changes are found, patients can pursue further testing or make lifestyle changes.
The images Smith generates each have about 50,000 pixels and the cameras can see 1/100 of a degree change from pixel to pixel.
What’s important, added Smith, is the temperature difference in the pattern on a pixel-to-pixel basis, not simply the change in colors apparent to the naked eye.
“Somebody might have more red on their follow-up visit or their annual visit, but that could be for a lot of reasons,” explained Smith. “They could be warmer or producing more estrogen because they’re taking hormones, or in a different place in their menstrual cycle.”
Reds are hotter, blues are colder and green, a neutral color, doesn’t have much meaning. A “hot spot” doesn’t necessarily mean cancer, nor is an area shaded in blue always good, said Smith.
Developing pathology like infections, fibrocystic breast disease, estrogen dominance or something more serious like cancer, said Smith, would change the thermal map. The scan can even detect inflammation from a tooth filling or from the carotid artery.
“We’re kind of like a GPS for your health,” said Smith. “If you’re starting to go in the wrong direction, we help you get back… We’re trying to help people stay healthy.”
Thermography serves as a screening for those who are healthy looking to stay on that course or for women who fall outside the recommended age group for mammograms, ages 40 to 70. The practice is used to monitor cell growth, but Smith is quick to note that this practice does not diagnose cancer.
In the case of breast cancer, it takes years for a mass to develop and be felt or seen on a diagnostic test. But thermography allows for the budding cells to be seen. That’s because the cancerous cells that are growing generate more heat.
Prevention trumps detection, said Smith.
“We want to be screening like we do with our cholesterol, where we can make changes and actually stay well,” said Smith. “Thermography is one more tool in the toolbox.”
To learn more about Dr. Hillary Smith’s practice, visit www.thebreastthermographycenter.com
Beth Roessner, The Desert Sun 5:38 p.m. PDT May 28, 2014